Pain relief in labour - natural techniques and pain medications for giving birth
26 methods for pain relief to help you bring your baby into the world


While some women are keen to make use of all available drugs to make labour pain-free, others won't want any. There is no one right path for any labouring mum and you can always change your mind. Whether you want to go with the flow and see how things happen or opt for pain relief from the start, it’s entirely up to you.
Bear in mind, that the pain relief options available to you in labour will depend on where you have your baby. If you’re giving birth in a hospital, you will have access to the full range of drugs for pain relief in labour. You can also use more holistic approaches, like relaxation techniques or water birth. If you’re giving birth in a midwife-led unit or at home, your options will be more limited. That’s because some pain relief drugs can only be given by a doctor. For example, an epidural can only be given by an anaesthetist at a hospital. However, some medicinal pain relief in labour, like gas and air, pethidine and morphine, can be prescribed by a midwife during a home birth or at a midwife-led unit.
To find out more about the different types of pain relief available to labouring women, we talked to consultant Simon Jones, an obstetric anaesthetist from Northumbria and Benash Nazmeen, a midwife in Sheffield.
Pain relief in labour
Back massage and a warm bath
Staying comfortable in the early stages of labour is important to help you relax and keep labour going. Bear in mind, that you’ll likely be without medical support at this time, as you’ll need to wait until your contractions are closer together before you head to the hospital (or your midwife arrives for a home birth). Many women find gentle back massage soothing for those initial labour aches and pains. A warm bath is also very relaxing and helpful for first contractions. Some labouring women describe these as feeling like period pains.
Mum of three Anna told us, “There’s something so soothing about stepping into warm water. As it envelops you, the weight of the water holds you like a hug and any movements you make are slow and steady. In water, there are very few restrictions on your movement like there can be on a bed. It’s the softness of it all really, which I think helps you to focus inwards and on what your body is able to do.”
It’s important to make sure that you call the midwife when your waters break. They will ask you to keep an eye on your labour timings and call back when contractions are close together and becoming more intense. You should also call for advice if your baby’s movements change, you’re unable to deal with the pain or if pain doesn’t fade away in between contractions. Smelly or discoloured waters or any vaginal bleeding also means an immediate call for assistance.
Breathing and relaxation techniques
Many women use relaxation techniques to “breathe through” their contractions and help them stay focused during early labour. Midwife Benash Nazmeen told us “Breathing and visualisation techniques are great for getting you in a calm state and feel like you have an awareness of what is happening for you. Guided relaxation can be helpful as well - so some people imagine flowers opening and flourishing to give them the idea of a sense of journey or progress as their contractions increase in intensity.”
Breathing techniques are one of the most common methods of pain relief. There’s not been a lot of research on how effective breathing techniques are for pain relief in labour. However, one study of 2,400 mothers, discovered 48 per cent found breathing techniques useful. Another study by Yuksel et al found breathing exercises reduced perceptions of pain and “recommend breathing exercises” for “pain management and shortening the duration of labour”.
Hypnobirthing
Hypnobirthing is the idea of using positive statements, (“affirmations”) with relaxation and “visualisations”. Hypnobirthing teachers recommend practising relaxation through pregnancy, so when labour starts, you can have a relaxed state of mind. It was originally developed by hypnotherapist Marie Mongon in the 1980s.
Midwife Benash told us, “Some people think that hypnobirthing is a bit airy-fairy and not for them. It's all about self-management and self-soothing. Relaxation techniques of hypnobirthing can stop you from going into the “fight or flight” reaction. This reduces the chance of adrenaline slowing down your labour. Not all techniques work for everyone. You can find out what works for you when using hypnobirthing to relieve pain in labour”.
Liza, mum of 5, who used hypnobirthing told us, “I simply imagined I was like a lotus flower as each surge or contraction happened. I knew I just had to get through each one and each powerful brought me closer to meeting my beautiful twins. I know that hypnobirthing helped me stay calm. The doctors didn’t realise how far I’d progressed until they noticed baby crowning. I seemed far calmer than they had expected”.
One of the largest studies on hypnobirthing for pain relief in labour was Werner et al’s 2013 study. This study found women using hypnobirthing rated labour as better than those who did not use the techniques.
A 2016 review of nine studies - taking into account the experiences of 3000 birthing women - found that women who did hypnobirthing were 27 per cent less likely to use drugs for pain relief. However, the researchers did not find a reduction in the use of epidurals and there wasn’t enough evidence to conclude it made a significant measurable difference in pain relief in labour.
Recommended hypnobirthing books
Written by Marie Mongan, this guide outlines the stages of labour and prepares mums-to-be with hypnotism and visualisation techniques to manage pain. With a 4.5 star rating on Amazon, it also offers advice on birthing positions and technical jargon.
Hypnobirthing coach Hollie de Cruz aims to provide mums with the skills they need to feel safe and empowered during birth. Having worked with Fearne Cotton and Giovanna Fletcher she shares advice on movement, breath and powerful visualisation techniques to manage pain.
Position and movement
Many TV shows and movies show labouring women on their backs, with their feet up in stirrups and a doctor waiting to catch the baby. In fact, around 68 per cent of women report giving birth in this position.
However, this position, (“lithotomy”) is one of the worst positions to give birth in. If you look at your anatomy, lying on your back angles your pelvis. This means your baby and you have to work against gravity.
Research on MRIs of pregnant women shows us that the pelvis is wider when squatting and on hands and knees than on the back.
The upright position in labour
A 2017 study reviewing positions for women in labour found the upright position:
- Made labour happen faster
- Reduced the need for assisted deliveries (using instruments to help birth)
- Meant fewer episiotomies (cuts to the vaginal area to assist birth)
However, these differences were quite small and the evidence was not found to be overwhelmingly strong. They concluded that more research is needed on the benefits of positioning in labour.
Birthing balls for position in labour
Many women find the use of large, inflatable birthing balls (Amazon | from £22.95) useful for pain relief during labour. Bouncing on the ball during pregnancy and early labour can:
- Be meditative
- Give your abdomen support
- Help with back pain
- Reduce overall labour pain
One Taiwanese study showed birthing balls help mothers with reducing pain and shorten labour. The study said birthing balls mean a “shorter first-stage labour duration [and] less epidural analgesia”.
A larger study also studied the evidence on birthing balls. It looked at 220 labours and discovered birthing balls:
- Reduced how much pain women experienced
- May help support the perineum (the area between the vaginal opening and anus)
- May increase the effectiveness of contractions
- Help gravity to enhance the movement of the baby through the vagina
- Decreases pain in the back
- Distracts labouring women from labour pain
- Promote comfort and relaxation
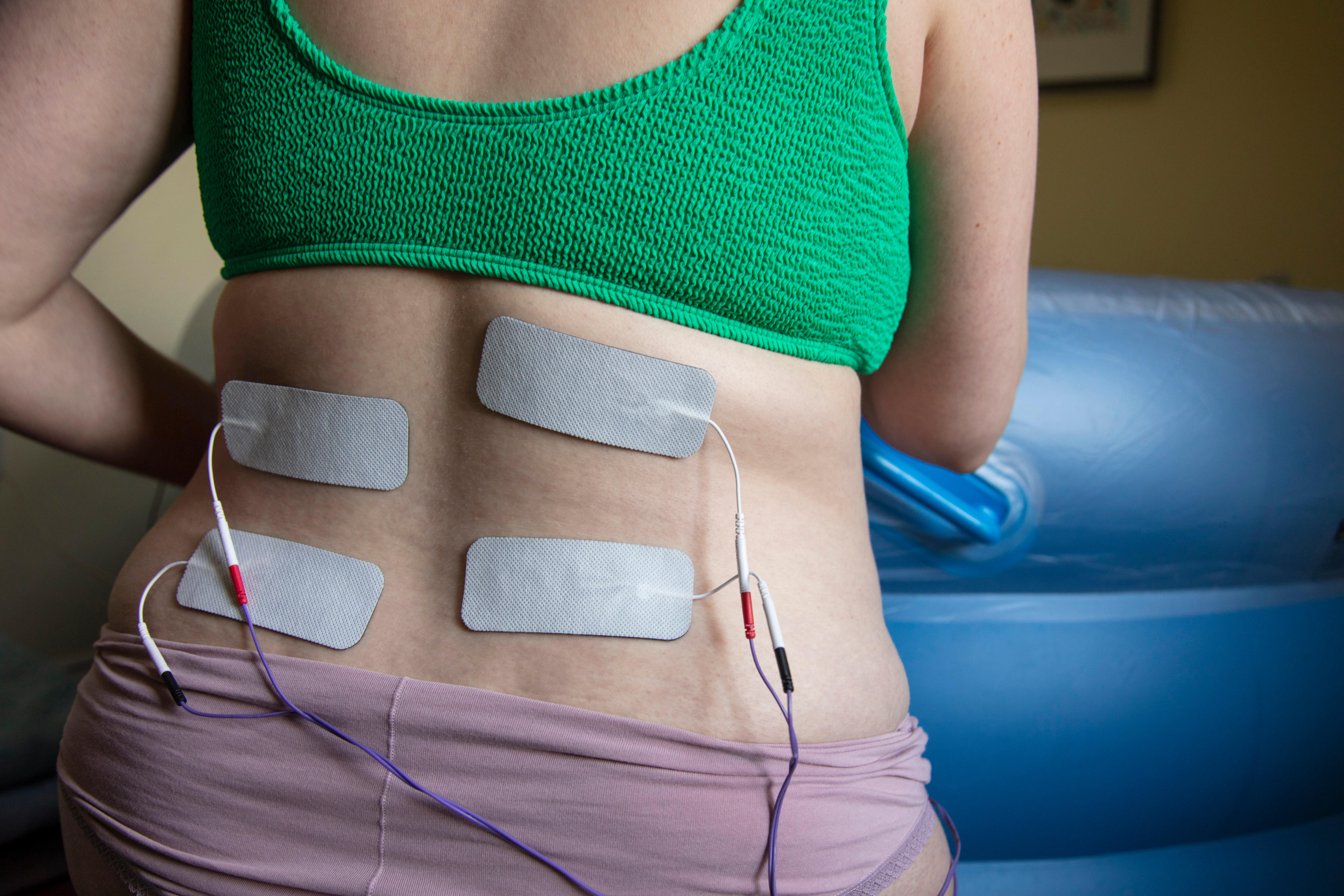
TENS machines for pain relief in labour
TENS (transcutaneous electrical nerve stimulation) machines (£29.99 | Boots) are a drug-free method of pain relief for pregnancy and labour. They use a small, battery-powered machine to deliver small amounts of electrical stimulation to nerves. The theory is that the electrical signals stimulate the natural painkilling response. This releases hormones called “endorphins”. These are often known as “feel-good” chemicals as they reduce pain and enhance mood.
When using a TENS machine you will feel a mild buzzing sensation and you can easily control the level and frequency of the machine.
You cannot use TENS machines in or near water, or with heat. They can be stopped or started at any time and can also be used during pregnancy without adverse effects on you or your baby.
One large study from 2017 concluded there was limited evidence that TENS machines provide any relief from pain in labour. Smaller studies, including research by Shahoei concluded TENS machines do reduce labour pain.
Waterbirth for pain relief in labour
Waterbirth was first recommended by the UK Department of Health for pain relief in labour in 1993. It’s become increasingly popular ever since. The Care Quality Commission’s 2019 survey showed 19 per cent of women used a birthing pool during labour.
There is a lot of research and evidence about both the safety and benefits for mother and baby when it comes to waterbirth:
- Many large studies of several smaller studies (a meta-analysis) show that waterbirth is as safe as “land birth”.
- One study conducted over 12 years, showed waterbirth reduced tears and postnatal bleeding.
- A major review of 15 studies looked at 3663 women’s labour in water, concluding that water birth reduces your likelihood of having an epidural.
- Research by Declercq et al. and a study by Eberhard et al concluded water birth was as effective for pain relief as opioids.
- A study by Gayiti and other research by Thoeni found water birth shortened labour and provided good pain relief.
- A study reviewing over 18000 water births concluded water birth is safe for mother and baby. Research on waterbirth has been shown to provide good pain relief in labour, meaning women ask for less pain relief (Nutter et al).
However, water birth is less common in America. In April 2021, the American College of Obstetricians and Gynaecologists stated they are against birthing in water.
The UK’s guidelines for women in labour recommend the use of water birth for pain relief in labour.
What should I do if I want a waterbirth?
If you decide you'd like to have a water birth, you should discuss this with your midwife. Depending on where you want to have your baby, you can have a water birth in hospital, a birth centre or even at home.
If you want a home birth in water, you will need to buy or arrange a pool rental. Some doulas provide birth pool rental services and your midwife may be able to recommend a reputable place to buy one.
Some mums enjoy birthing in a pool that other local babies have been born in. If you're using a preloved birthing pool, you will need to buy a birthing pool liner (Universal Pool Liner, Home Birth Supplies| £27.99).

Pain medications in labour
Gas and air
Gas and air, also known as Entonox, is one of the most common forms of pain relief used during labour. It is safe for both mother and baby. Composed of 50 per cent oxygen and 50 per cent nitrous oxide, midwives don’t need a doctor to prescribe it. You can use gas and air when birthing at home, in a midwife-led unit or in a hospital. Consultant in Obstetric anaesthetist, Dr Simon Jones told us, “Gas and air is one of the most common forms of pain relief in labour. Some people get through all of labour using it but it relies on a good technique. Timing its use with contractions is important for maximum effectiveness”.
Nitrous Oxide is the active ingredient and works when you inhale it. Similar to opioid painkillers, research shows it works on receptors in the brain to reduce pain sensitivity and perception. In the UK, the most recent CQC report reveals gas and air is the most popular form of pain relief in labour: 77 per cent of women use it when giving birth.
Pros of gas and air
- short-acting, meaning the effects do not last very long (seconds to minutes)
- many women like the sense of control over their pain
- Stop taking it when you wish
- No impact on labour progression
- No impact on the baby
- Very effective and fast at relieving pain
- You can use gas and air wherever you choose to give birth
- No need for extra monitoring
Cons of gas and air
- Can make you feel sick
- May dry out your mouth
- There are major concerns about the effects of nitrous oxide on the environment. Research reveals it can impact the ozone layer. The report suggests "nitrous oxide (gas and air) used by women today during labour will remain in the atmosphere for more than 100 years."
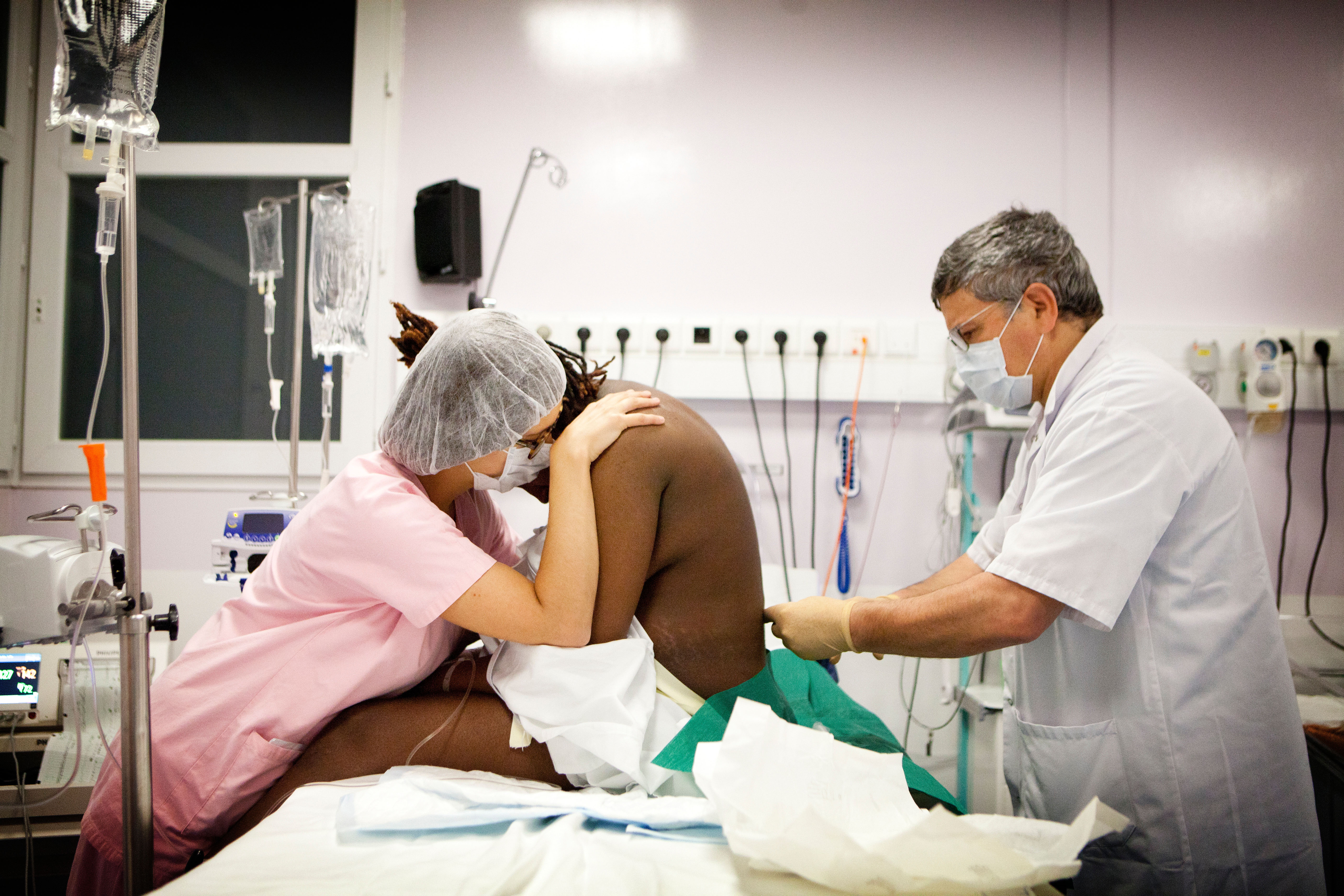
Epidural for pain relief in labour
Safe and effective, epidurals have been around since the early 1920s, when Spanish doctors first described anaesthetic injection into the “epidural space”. This area is filled with cerebrospinal fluid, just outside the spine’s nerves.
Having an epidural is when a fine tube (catheter) is placed in your back. Through this tube, local anaesthetic and painkillers are delivered to your spinal cavity. The epidural catheter will remain there for the duration of labour. It takes about 5-10 minutes for the anaesthetist to do. Epidurals are what Consultant Anaesthetist Dr Simon Jones calls “the gold standard” in pain relief for labour.
As epidurals are complicated, they can only be performed by a highly trained anaesthetist in a hospital. It's recommended you ask for an epidural early in labour, because it can be more difficult to put in as contractions get stronger.
Pros of epidural for pain relief in labour
- Studies show an epidural is the most effective form of pain relief in labour
- Quick to place, it has a relatively fast onset of pain relief in labour
- Limited side effects - they will not make you feel sick or drowsy
- Usually no effect on the baby
- No higher risk for caesarean
Cons of epidural for pain relief in labour
- You may need to have your baby's heart rate monitored
- An epidural will limit your movement
- Can cause low blood pressure
- Epidurals can cause an increase in your temperature
- You can have difficulty passing urine
- 1 in 100 women will experience a severe headache in labour
- Some women may experience temporary (1 in 1000 women), and severe or permanent nerve damage (1 in 24,000 women). Yet this evidence suggests this is rare.
- Can make it harder for you to push during labour
- Might not work well (1/10 times it may need replacing)
- Can be harder to place in women with a high BMI
- Research shows epidurals can increase the length of labour
Pain-relieving opioid drugs
There are a few different opioid drugs that may be offered to you during labour. Not all drugs are available at all hospitals. It may depend on your local health authority which drugs you are offered. Opioid painkillers all work in a similar way - they block the pain receptors in your brain.
Given as an injection into your muscle, opioid painkillers can be given by a midwife and common ones used in labour are morphine, diamorphine and pethidine. These drugs are not available if you are giving birth at home.
Obstetric anaesthetist Dr Jones says that opioids might not be right for everyone as pain relief in labour. “For some women, these medicines can make them feel like they’ve had a bit of a ‘funny turn’. They can act as a sedative, though diamorphine is less likely to do that. Diamorphine is more popular for that reason - it is a purer version of the drug and it’s more predictable in terms of its side effects”.
Pethidine is commonly used as pain relief in labour. However, this drug can have an effect on the baby's ability to breathe and feed. That's why it is best used in the earlier stages of labour. Most opioid drugs can be used alongside gas and air. However, if your baby is affected, don't worry as the doctors will be prepared for this and will help your baby with any extra support they need.
Pros of opioid injections
- Opioids can help you relax and relieve anxiety
- Most opioids do not affect the baby when given at the right time in labour
- Effects are usually quick, but short-acting
Cons of opioid injections
- Some studies have found that opioids are less effective than gas and air and
- Research reveals that Pethidine only has a modest effect
- Diamorphine has been rated as a ‘poor’ painkiller in some studies
- They can make you feel sleepy or sick
- Opioids may slow your breathing
PCIA: Patient-controlled intravenous analgesia (remifentanyl or fentanyl)
If you cannot have an epidural, you might be offered Patient-Controlled Intravenous Analgesia. This might be called PCIA by your doctor or just "Remi".
The drugs used in this type of painkiller are very strong opioids. You will have a needle in your hand, attached to a pump. When you feel pain you can press a button to request a “top-up” of the drug.
Remifentanyl is the most powerful of the opioid drugs available in labour.
Dr Jones, an expert Obstetric Anaesthetist, says "It can disconnect you from the experience of labouring and make you very drowsy, so it’s not right for every labouring woman”.
Remifentanyl is very potent and has a powerful effect. That's why it's not right for everyone. Research shows it’s short-acting, lasting for a contraction or two, but it is incredibly strong. You need strict, one to one care and sometimes oxygen is needed to help you breathe. This is because there is limited evidence it can impact on the mother's breathing.
If you do need to use it, because you can't have an epidural, you will be monitored very carefully by a team of professionals. There's no shame in needing such a strong painkiller, especially if you have a medical condition that means you will need it to help you give birth.
Pros of remifentanyl/fentanyl PCIA
- You control the amount of pain relief given
- Can be used with gas and air
- Works very quickly and is very strong
- Useful if you cannot have an epidural, but need strong pain relief
Cons of remifentanyl/fentanyl PCIA
- It may affect the baby when it is born (slow breathing)
- Baby might find first feeds difficult
- Monitoring for the baby during labour might be required
- Extra oxygen may be needed
- It can make you feel sleepy or sick
- May increase the need for forceps
What’s the best method of pain relief in labour for me?
Many women start labour with a clear idea of what they want from pain relief in labour. Others decide to simply “go with the flow” and see what pain relief in labour they need at the time.
Whatever you decide during planning, it’s important to understand things can change. Whether it’s your first labour or even your third or fourth baby, every labour is different. It’s common to change your mind as time goes on. Your medical team will always support you in your decision.
Some women decide they want to have a drug-free labour, and then find they struggle with pain. Remember that it is not a competition. There are no prizes for getting through labour without drugs. It’s really ok to change your mind at any time. Don’t feel like you’ve ‘failed’ if you decide that labour is too painful. Every baby and every mother’s labouring experience is different. Even if you sailed through previous birth experiences, it doesn’t mean you can’t accept pain relief now.
What the experts want you to know about pain relief
Many pain relief options during labour are fast-acting and can provide almost instant relief. Consultant anaesthetist Simon Jones does recommend asking for an epidural early. It is far harder to do an epidural when contractions increase in frequency and strength.
Simon Jones, Consultant Anaesthetist told us: “Seeing a mum who wants an epidural at the last minute isn’t ideal and it can make putting one in really challenging, meaning it’s less likely to be effective. No one will judge you for changing your mind. It’s worth considering the pros and cons of each option so you can give truly informed consent. Start small and work your way up, until you feel your pain relief during labour is well managed.”-
Midwife Benash Nazmeen says: “Making a calming environment, wherever you are birthing is essential. This will help you control your pain relief in labour. You need to cocoon yourself. Turn the lights down and have a holistic approach to comfort. Take care of all your senses and trust your birth partner to advocate for you. Ask lots of questions during pregnancy and in labour to get that sense of control. Use a range of pain relief methods during labour to find what is right for you”.
Every woman’s experience is different and whatever you choose will be the right decision for you at the time. What's important is being aware of all the pros and cons. You should talk to your birth partner about what you do and don’t want to be offered during labour, and always be prepared to change your mind.
Michelle, who had two epidurals, said “I had an epidural and I was able to relax and rest and then my labour progressed without issue. I had another epidural in my second labour without hesitation and it was great, enabled me to rest.”
Hannah, who has a two year son, said “I only wanted gas and air because I was really curious what contractions felt like and wanted to experience them. Also I didn't really want an epidural. The thought of having to keep still while in pain was much much scarier to me than the thought of being in pain.”
Which pain relief in labour will I have access to?
Your pain relief in labour options will depend on where you choose to give birth.
Remember, your pain relief choices are flexible and you can change your mind at any point. Midwife Benash told us, “There are a lot of tools in your kit. Pain relief during labour relies on staying calm, so the only tension there should be is in your uterus, during contractions. Use things that make you happy to create that calming environment and use all of your senses to comfort and ground you. Concentrating on the pain or discomfort can amplify it. You won’t feel it as intensely if you’re able to focus and use your own self-soothing techniques alongside any medications you might want. Find what works for you to allow you to be calm and as relaxed as possible to meet your baby”
| Pain relief option | Home birth | Midwife-led unit | Labour and delivery suite |
| Self-help methods (e.g. hypnobirthing, position and movement, relaxation and breathing techniques) | ✅ | ✅ | ✅ |
| Waterbirth | ✅ (Buy or hire pool or use the bath) | ✅ (where available) | ✅ (where available) |
| Gas and air | ✅ | ✅ | ✅ |
| TENS machine (buy or hire your own) | ✅ | ✅ | ✅ |
| Opioid drugs (pethidine, morphine) | ❌ | ✅ | ✅ |
| Epidural | ❌ | ❌ | ✅ |
Video of the Week: Old wives' tales to predict the sex of your baby
Parenting advice, hot topics, best buys and family finance tips delivered straight to your inbox.

Tannice Hemming has worked alongside her local NHS in Kent and Medway since she became a parent and is now a mum of three. As a Maternity Voices Partnership Chair, she bridged the gap between service users (birthing women and people, plus their families) and clinicians, to co-produce improvements in Maternity care. She has also worked as a breastfeeding peer supporter. After founding the Keep Kent Breastfeeding campaign, she regularly appears on KMTV, giving her views and advice on subjects as varied as vaccinations, infant feeding and current affairs affecting families. Two of her proudest achievements include Co-authoring Health Education England’s E-learning on Trauma Informed Care and the Kent and Medway Bump, Birth and Beyond maternity website.



