Pre-eclampsia symptoms, risks, complications and treatments
Pre-eclampsia affects 1 in 10 pregnancies. Our in-depth guide will help you recognise signs and know how and when to get help

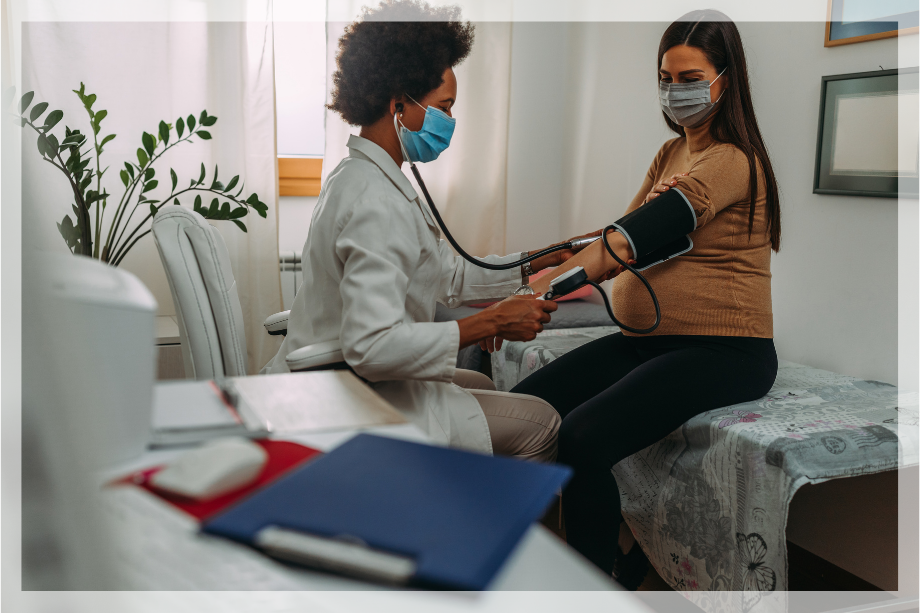
Pre-eclampsia symptoms usually develop in the second half of pregnancy at any time after 20 weeks, though it can occur earlier than that, at around 12 weeks.
Although most cases are mild, one pregnancy in 100 is so severely affected that there's a serious risk to the life of the baby - and even the mother. Pre-eclampsia is a condition that affects the placenta and can lead to high blood pressure. Some women don't have any pre-eclampsia symptoms at all. That's why it's important that you attend your routine antenatal appointments, so your midwife can look for signs of pre-eclampsia and test your urine.
Dr Anita Bannerjee, trustee of the UK charity, Action on Pre-Eclampsia (APEC) told us, "Pre-eclampsia symptoms are often a spectrum. Some mums don't even know they have it. It's a multi-system disorder, that can affect all kinds of things, including your liver, brain, eyes, heart, and kidneys. Blood tests can show it too. If you're experiencing odd symptoms or just don't feel well when you're pregnant, get checked out. It could be pre-eclampsia."
Pre-eclampsia symptoms
The main pre-eclampsia symptoms are:
- High blood pressure (higher than 140/90 mmHg)
- Protein in your urine
Protein is excreted in urine when you have pre-eclampsia because your kidneys aren't working properly. For some women, these are their only symptoms, especially if pre-eclampsia is caught early. Your midwife will check your urine during your routine antenatal appointments.
Other symptoms can include:
- Headaches and flashing lights
- Being short of breath
- Pain in your upper right quadrant (underneath your ribs)
- Blurred vision
- Vomiting
- Swelling in your hands, feet or face
Dr. Banerjee, from Action on Pre-eclampsia (APEC), told us: "Pre-eclampsia symptoms vary quite a lot. If you have a headache that you can't explain or see flashing lights - almost like lightning flashes - then seek immediate medical assistance. You might also have blurred vision. Headaches in pre-eclampsia are caused by oedema (swelling) in your brain. Pain under your ribs on the right side is also a cause for concern. That's usually a sign of liver trouble which can be caused by pre-eclampsia."
Parenting advice, hot topics, best buys and family finance tips delivered straight to your inbox.
The role of the placenta in pre-eclampsia - The placenta is an organ responsible for keeping your baby happy, healthy, and growing. As the only temporary organ, you make a new placenta for every baby. The placenta is "born" on the same day your baby is. The placenta is one of the organs that science understands the least. As the latest studies show, the placenta filters toxins from your blood and provides nutrition and a blood supply to your baby. Waste products from your baby go back into the placenta for the mother's body to excrete.
In pre-eclampsia, there is a problem with the placenta. Studies show this is usually caused by malperfusion, which means it's not getting sufficient blood supply. The damaged placenta causes high blood pressure because it affects blood vessels. Restricted blood flow between you and your placenta can result in a reduced supply of oxygen and nutrients to your baby. This may mean that he/she doesn't continue to grow as well as expected.
Because there is no cure for pre-eclampsia other than delivery, many babies have to be induced prematurely and sadly not all survive.
Who is at risk of pre-eclampsia?
- Family history: if pre-eclampsia affected your mother or sister (or your partner's mother or sister)
- This is your first pregnancy
- You are a young mum
- If you are an older mum
- Your BMI in pregnancy (or your partner's BMI) is higher than average
- If you have other conditions including diabetes, gestational diabetes) or kidney problems
- Having had pre-eclampsia in your previous pregnancies
- You are expecting two or more babies
- A long gap (10 years plus) between pregnancies
Some women have more potential risk factors for pre-eclampsia than others. The average pregnant woman has a 4-8% risk of pre-eclampsia, according to research by King's College London. Studies also show the risk of 4.1% in first pregnancies, drops to 1.7% in later pregnancies.
How does the father cause pre-eclampsia?
If you have a large gap between pregnancies, of 10 years or more, you are more at risk. The reasons for this are unclear - but it may be because you're more likely to have a new partner. According to research, a new partner can raise your risk of pre-eclampsia. Like your baby, the placenta is formed of 50% DNA from your partner and 50% from you. If your partner's mother had pre-eclampsia in any of her pregnancies, it can increase your risk, too. It's estimated that around 13% of pre-eclampsia cases are caused by factors contributed by the baby's father.
Pre-eclampsia treatments
Giving birth is the only cure for pre-eclampsia. However, it is possible to manage some pre-eclampsia symptoms during pregnancy, to give your baby a little more time to develop.
Medication can also help mothers with pre-eclampsia:
- Control blood pressure (antihypertensive medications)
- Prevent seizures (anticonvulsants)
Dr. Banerjee explains: "Every woman's experience is different and treatment depends on you, your general health, and your baby. Whether or not you need to deliver early will depend on how unwell you are and how your baby is doing. Your doctors will explain everything to you and reassure you about what will happen next."
How will pre-eclampsia affect my birth?
At some point concerns about your safety and/or that of your baby may mean that labour needs to be induced. Given your condition and the nature of an induced birth, it does mean that you and your baby will require extra monitoring during labour and you may not be able to have the type of labour and delivery you had hoped for. However, most women with pre-eclampsia do have vaginal deliveries. If your baby is being born prematurely then the special baby care team will be on full alert.
Premature birth happens before 37 weeks.
Early delivery indications include:
- Liver or kidney function is poor in the mother
- There is placental abruption (the placenta has come away from the womb wall)
- You have uncontrolled blood pressure, despite treatment with medication
- Severe headaches or seizures indicate a risk of neurological damage
(Source: NICE guidelines, UK)
For further information, read our advice on what happens if you’re diagnosed with pre-eclampsia?
Pre-eclampsia complications
Pre-eclampsia can be fatal for mum and baby, in rare cases. In some countries with poor antenatal care, it is the leading reason for maternal death. This usually occurs when pre-eclampsia is diagnosed late.
According to Action on Pre-Eclampsia, other rare potential complications from pre-eclampsia can include:
- Stroke
- Seizures or convulsions
- Placental abruption (where the placenta separates from the wall of the womb during pregnancy)
- Reduced fetal movements (if you notice your baby isn't moving as often as usual, please immediately contact your maternity assessment unit)
- Reduced fetal growth (Intrauterine growth restriction) caused by poor blood supply from the placenta
- Lower birth weight, is caused by the reduced nutrition caused by a poorly functioning placenta
- HELLP syndrome in the mother (a disorder that affects the liver and blood clotting disorder)
"Pre-eclampsia is usually mild, but 1-2 in every 100 first pregnancies is so severely affected that there is a serious risk to the life of the baby – and even the mother. Every year in the UK about 1000 babies die because of pre-eclampsia – many of these as a consequence of premature delivery rather than the disease itself. Some 1-2 mothers die each year from complications of pre-eclampsia in the UK." - Action on Pre-Eclampsia
These rare risks are very uncommon in the UK. The UK's good antenatal care means most cases of pre-eclampsia are diagnosed early. The majority of women with pre-eclampsia won't suffer from any of these rarer complications. So don't panic if you think you might have pre-eclampsia. Most women don't develop pre-eclampsia until the third trimester when they're already closer to delivery.
Regular checks for pre-eclampsia
You will be monitored throughout your pregnancy for pre-eclampsia symptoms. At your initial booking appointment with your midwife, your risk factors will be identified and discussed with you. Never miss an appointment and if you do have to cancel one, reschedule for as soon as possible.
If you are at higher risk, then it's important to be vigilant. Listen to your own body and if you're feeling really unwell with any of the symptoms described above then don't ignore them and don't be fobbed off with the explanation that they're simply the common side effects of a normal pregnancy. They may not be. It's important to voice any concerns you have and be assertive.
Dr Banerjee told us, "We have to empower every mother to ask for blood pressure and urine checks at every appointment. Noticing pre-eclampsia before it starts to affect you is so important. Go to your appointments with your urine sample if you can. Don't miss an opportunity to make sure your placenta is functioning as it should."
Ann Marie Barnard, (now the former) chief executive of the charity Action on Pre-eclampsia also told us, "In my experience women usually do know when something is wrong but sometimes they need to be a lot more assertive. I know this is often hard, particularly when you are pregnant and maybe feeling a bit vulnerable. But so many times I have women say to me, 'I knew that something wasn't right but no one would listen to me'. If you're worried that no one is listening to you and you find it hard to make a fuss then take someone with you who can be your advocate and spokesperson."
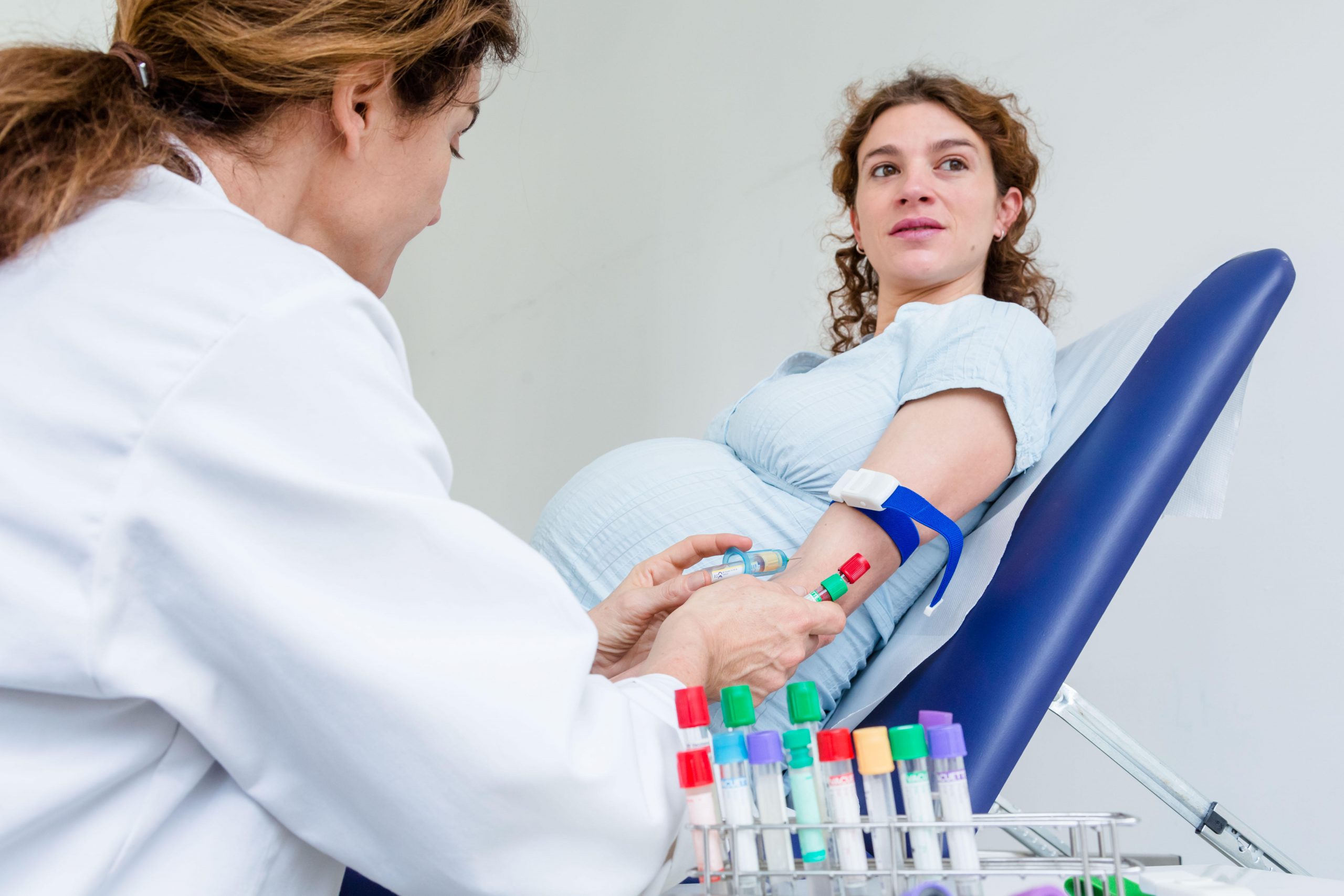
Postpartum pre-eclampsia: what are the symptoms after delivery?
Rarely, women can develop pre-eclampsia after they have given birth. Known as postpartum preeclampsia, most cases of postpartum pre-eclampsia happen 48 hours after birth. However, late postpartum pre-eclampsia can develop up to 6 weeks after the baby's birth.
Symptoms of postpartum pre-eclampsia are the same as pre-eclampsia during pregnancy. These include:
- High blood pressure
- Decreased urination
- Pain under your ribs (on the right side)
- Headaches or changes in your vision
- Nausea and/or vomiting
- Shortness of breath
(Source: APEC UK)
If you experience any of these in the period after giving birth, seek immediate medical assistance. More advice on postpartum eclampsia is available from Action on Pre-Eclampsia's Postpartum Pre-Eclampsia info leaflet.
How to prevent pre-eclampsia
Of course, it's not possible to prevent all of the risk factors that can affect your chances of developing pre-eclampsia in pregnancy. You can't change your (or your partner's) family history.
There's also not a lot of good quality evidence demonstrating ways to prevent pre-eclampsia with lifestyle changes - before or during pregnancy. Some doctors have concluded, "In developed countries, the majority of cases [...] are considered unpreventable".
Lifestyle changes - Various studies suggest there is no evidence that any changes to diet or lifestyle have an appreciable effect on the chances of developing pre-eclampsia. However, of course, we all know the importance of a good diet when it comes to preventing other illnesses in pregnancy, like gestational diabetes.
However, supplementation of calcium and vitamin D in pregnancy has been shown to improve outcomes in women with low calcium. When your midwife does regular antenatal blood tests, they will be able to identify any supplements you should take.
Medication - Current guidelines in the UK recommend the use of aspirin for those considered at moderate or high risk of pre-eclampsia. The recommended dose is 75–150 mg of aspirin daily. Your doctor will suggest you take it from 12 weeks until your baby is born. (NICE, UK)
Obstetric Medicine doctor Dr. Banerjee told us, "Many women feel quite guilty about taking medications in pregnancy. However, there is really good, high-quality evidence that low-dose aspirin is effective for preventing pre-eclampsia. Some evidence has shown it's better if you take it at night. If you have concerns about your risk of pre-eclampsia, have a discussion with your midwife. Your healthcare team can explain if preventative aspirin is right for you".
To find out more about pre-eclampsia symptoms, risks, and treatments for the condition, we talked to Dr Anita Bannerjee, trustee of the UK charity, Action on Pre-Eclampsia (APEC). Dr. Banerjee is also an Obstetric Medicine doctor at King’s College London. She is also the Deputy Director of Medical Education at Guys and St Thomas’ Hospitals NHS Foundation Trust.
You might also like:
The stages of labour and birth, according to a midwife
Braxton Hicks contractions: Your questions answered
Contractions in pregnancy - different types and what they mean
Early signs of labour: How to tell if your baby is coming
Video of the Week:

Tannice Hemming has worked alongside her local NHS in Kent and Medway since she became a parent and is now a mum of three. As a Maternity Voices Partnership Chair, she bridged the gap between service users (birthing women and people, plus their families) and clinicians, to co-produce improvements in Maternity care. She has also worked as a breastfeeding peer supporter. After founding the Keep Kent Breastfeeding campaign, she regularly appears on KMTV, giving her views and advice on subjects as varied as vaccinations, infant feeding and current affairs affecting families. Two of her proudest achievements include Co-authoring Health Education England’s E-learning on Trauma Informed Care and the Kent and Medway Bump, Birth and Beyond maternity website.